IRANDERMA |
|
Quiz: December 2009 |
What is your diagnosis for this 4-year-old boy?
He has had this solitary enlarging tumor on his chin since about 6 months ago. Histopathological examinations revealed a non-capsulated tumor composed of spindle cells arranged in fascicles. The tumor has hemoangiopericytic-like vascular structures. No significant mitotic activity or necrosis is identified. Immunostaining was positive for smooth muscle actin and negative for desmin and CD34.
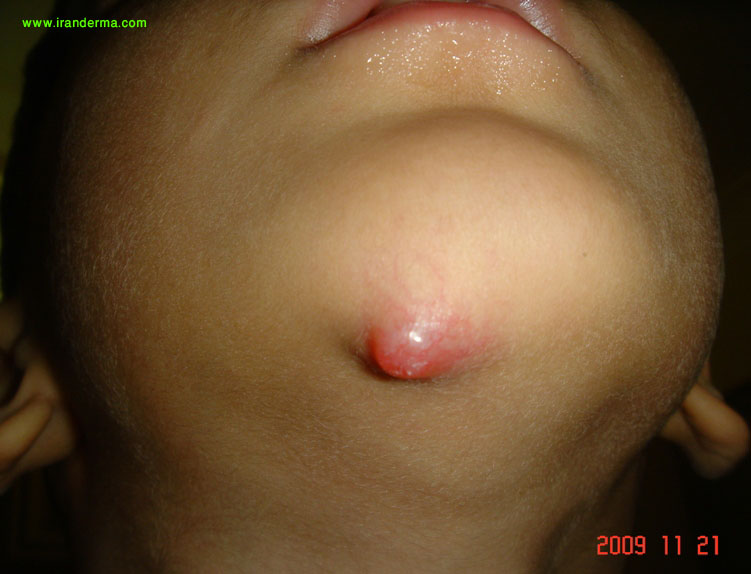
Diagnosis: Nodular fasciitis
Omid Zargari, MD, FAAD:
Nodular Fasciitis(NF) is a benign reactive tumor presenting as a rapidly growing subcutaneous nodule.
This tumor is seen mostly in young to middle-aged adult s. In children, the head and neck region is the most common site.
Reza Ghaderi, MD:
Nodular faceitis is a benign proliferation of fibroblasts and myofibroblasts in the subcutaneous tissues. The lesions are generally small and solitary, arising commonly in the upper extremities of adults and in the head and neck region of infants and children. A history of trauma may precede these reactive lesions, but their cause is unknown.
Physicians are often called upon to do excisional biopsies in the diagnosis of subcutaneous tumors. Benign fibrous tumors represent a group of clinical entities that are often difficult to diagnose. NF is one such benign fibroblastic proliferation whose rapid growth and rich cellularity frequently cause the lesion to be misdiagnosed as sarcoma.
NF was first described by Konwaler in 1955 and was termed pseudosarcomatous fibromatosis. Other terms, such as pseudosarcomatous fasciitis, infiltrative fasciitis, and proliferative fasciitis, have also been used synonymously.
The incidence of nodular fasciitis is unknown. It is possible that the lesion's true incidence has been obscured by prior misdiagnosis as malignancy.
Nodular fasciitis is most commonly seen in young adults between 30 and 40 years of age. Approximately 10 percent of the lesions occur in children. Men and women appear equally affected, although in childhood the lesions may occur predominantly in boys. Most patients with this reactive proliferation have a rapidly growing mass. In several reports, nearly half the patients had noted the growth for less than a month. More than one third of patients report pain or tenderness associated with the lesion.
Diagnosis of NF requires histologic confirmation, and both diagnosis and treatment are accomplished by excisional biopsy.
Differential diagnosis:
A. Benign
tumours:
1.Benign
fibrous histiocytoma-
Classical -Epidermal
hyperplasia, peripheral
collagen bundles, foamy
macrophages and Touton
giant cells . Cellular
variant- Fascicular
spindle cell
architecture.
2.Neurofibroma-
Architecture is
different, S100 protein
is positive
3.Spindle
cell lipoma
- Fat, ropy collagen,
absence of markers
4.Fibromatosis-
More infiltrative growth
pattern, slender spindle
shaped fibroblasts
arranged in sweeping
fascicles and separated
by abundant
intercellular collagen.
B. Malignant
tumours:
1.
Leiomyosarcoma-
The cells in fasciitis
are tapered and the
nuclei are tapered
rather than blunt
ended. Atypical mitotic
figures are
prominent.Immunohistochemistry
reveals h-caldesmon and
desmin positivity.
2. Low
grade myofibrosarcoma (myofibroblastic
sarcoma)
shows focal nuclear
atypia,less
inflammation, more
uniformly cellular,
reaches a larger size
and infiltrates muscle.
3.
Inflammatory
myofibroblastic tumour
has
fasciitis-like,fascicular
and fibrous areas and a
marked plasma cell
infiltrate.
Immunohistochemistry
reveals that some cases
are cytokeratin and
ALK-1 positive.
4. Myxoid
malignant fibrous
histiocytoma
is multinodular ,has
vacuolated fibroblasts
and shows nuclear
pleomorphism, abnormal
mitosis, distinct
vascular pattern and is
usually actin negative
(some are CD34
positive).
5.
Malignant peripheral
nerve sheath tumour
has alternating cellular
and myxoid fascicles, is
more uniform and has
wavy buckled and bullet
shaped nuclei. Better
differentiated case are
at least focally
S100 protein positive
and myoid markers are
negative.
The following features
rule out malignant
tumour:
1. Absence of
atypia 2. Absence of
atypical mitotic
figures 3.Small size
4.Short history
5.Superficial location
in young adults.
Variants:
1. Ossifying
fasciitis: Nodular
fasciitis like
fibroblastic
proliferations with
metaplastic bone
formation.
2. Intravascular
fasciitis: Involve small
or medium-sized veins or
arteries. Histologically
the features are similar
to nodular fasciitis,
however there are
greater number of
multinucleate giant
cells and less prominent
mucoid matrix.
3.
Cranial fasciitis: The
lesion involves the soft
tissue of the scalp land
is usually present in
infants. Histologically
this is well
circumscribed lesion
showing NF like
fibroblastic
proliferation in a
prominent myxoid stroma.
These lesions rarely recur, do not develop metastases, and are readily cured by local excision. Spontaneous regression of incompletely excised lesions of NF has also been reported. Once the diagnosis is made by excisional biopsy, no further treatment appears necessary.
ايران درما |